| Video Discription |
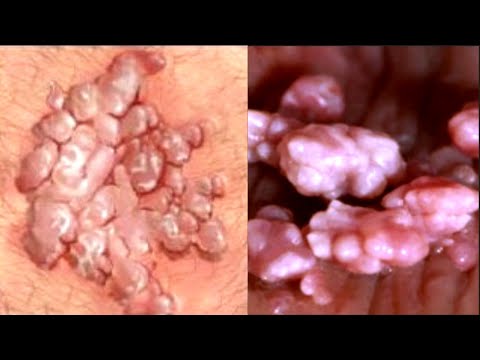
REMOVAL OF ANO –PERIANAL WARTS
• Anogenital warts are a common disease, and 90% are caused by nononcogenic HPV types 6 or 11.
• Can be associated with foci of high-grade squamous intraepithelial lesion (HSIL), particularly among persons who have HIV infection.
• us, which is predominantly transmitted by skin-to-skin or mucosa-to-mucosa contact
•
• Anogenital warts are usually asymptomatic; however, depending on the size and anatomic location, they can be painful or pruritic. They are usually flat, papular, or pedunculated growths on the genital mucosa.
• Intra-anal warts are observed predominantly in persons who have had receptive anal intercourse; however, they also can occur among men and women who have no history of anal sexual contact.
• Diagnosis of anogenital warts is usually made by visual inspection but can be confirmed by biopsy, which is indicated if lesions are atypical (pigmented, indurated, affixed to underlying tissue, bleeding, or ulcerated lesions).
• Some anogenital lesions (condyloma accuminata) can resemble anogenital warts but do not respond to anogenital wart treatment. Condyloma lata, a manifestation of secondary syphilis, can be diagnosed by serologic tests or through direct detection from serous fluid from the lesions.
• The aim of treatment is removal of the warts and amelioration of symptoms, if present.
• The appearance of warts also can result in considerable psychosocial distress, and removal can relieve cosmetic concerns.
• If left untreated, anogenital warts can resolve spontaneously, remain unchanged, or increase in size or number.
• Because warts might spontaneously resolve in 1 year, an acceptable alternative for certain persons is to forego treatment and wait for spontaneous resolution.
• Treatment of anogenital warts should be guided by wart size, number, and anatomic site; patient preference; cost of treatment; convenience; adverse effects; and provider experience.
• Persons with external anal or perianal warts might also have intra-anal warts. Thus, persons with external anal warts might benefit from an inspection of the anal canal by digital examination, standard anoscopy, or high-resolution anoscopy.
In addition to anogenital warts, HPV types 6 and 11 have been associated with conjunctival, nasal, oral, and laryngeal warts.
• Treatment regimens are classified as either patient-applied or provider-administered modalities. Patient-applied modalities are preferred by certain persons because they can be administered in the privacy of their home.
• the Human Papilloma Virus (HPV) used to be thought of as one of the most common sexually transmitted diseases (STDs) . However, penetrative sexual contact is not in fact necessary to transmit the virPodofilox (podophyllotoxin) is a patient-applied antimitotic drug that causes wart necrosis.
• Podofilox solution (using a cotton swab) or podofilox gel (using a finger) should be applied to anogenital warts 2 times/day for 3 days, followed by 4 days of no therapy.
• This cycle can be repeated, as necessary, for up to four cycles.
Podophyllin 20-25% is inexpensive, but it is mutagenic and only moderately efficacious. Recommended treatments that can be used in the doctor's office include trichloroacetic acid or physical ablation using cryotherapy, electrosurgery, excision, or laser treatment.
• Cryotherapy is a therapy that destroys warts by thermal-induced cytolysis.
• A correct use of this therapy is essential because overtreatment or under treatment can result in complications or low efficacy.
• Pain during and after application of the liquid nitrogen, followed by necrosis and sometimes blistering, is common.
• Fewer data are available regarding the efficacy of alternative regimens for treating anogenital warts, which include podophyllin resin, intralesional interferon, photodynamic therapy, and topical cidofovir.
• Anogenital warts have decreased among adolescents, young women, and heterosexual men with use of HPV vaccination in multiple countries. |